2 results
Antiviral and Anti-Inflammatory Activities of Fluoxetine in a SARS-CoV-2 Infection Mouse Model
- D. Péricat, S. A. Leon-Icaza, M. Sánchez-Rico, C. Mühle, I. Zoicas, F. Schumacher, R. Planès, R. Mazars, G. Gros, A. Carpinteiro, K. A. Becker, J. Izopet, N. Strub-Wourgaft, P. Sjö, O. Neyrolles, B. Kleuser, F. Limosin, E. Gulbins, J. Kornhuber, E. Meunier, N. Hoertel, C. Cougoule
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S119-S120
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The coronavirus disease 2019 (COVID-19) pandemic continues to cause significant morbidity and mortality worldwide. Since a large portion of the world’s population is currently unvaccinated or incompletely vaccinated and has limited access to approved treatments against COVID-19, there is an urgent need to continue research on treatment options, especially those at low cost and which are immediately available to patients, particularly in low- and middle-income countries. Prior in vitro and observational studies have shown that fluoxetine, possibly through its inhibitory effect on the acid sphingomyelinase/ceramide system, could be a promising antiviral and anti-inflammatory treatment against COVID-19.
ObjectivesThe aim of this sudy was to test the potential antiviral and anti-inflammatory activities of fluoxetine against SARS-CoV-2 in a K18-hACE2 mouse model of infection, and against several variants of concern in vitro, and test the hypothesis of the implication of ceramides and/or their derivatives hexosylceramides.
MethodsWe evaluated the potential antiviral and anti-inflammatory activities of fluoxetine in a K18-hACE2 mouse model of SARS-CoV-2 infection, and against variants of concern in vitro, i.e., SARS-CoV-2 ancestral strain, Alpha B.1.1.7, Gamma P1, Delta B1.617 and Omicron BA.5.
ResultsFluoxetine, administrated after SARS-CoV-2 infection, significantly reduced lung tissue viral titres (Figure 1) and expression of several inflammatory markers (i.e., IL-6, TNFα, CCL2 and CXCL10) (Figure 2). It also inhibited the replication of all variants of concern in vitro. A modulation of the ceramide system in the lung tissues, as reflected by the increase in the ratio HexCer 16:0/Cer 16:0 in fluoxetine-treated mice, may contribute to explain these effects (Figure 3).
Image:
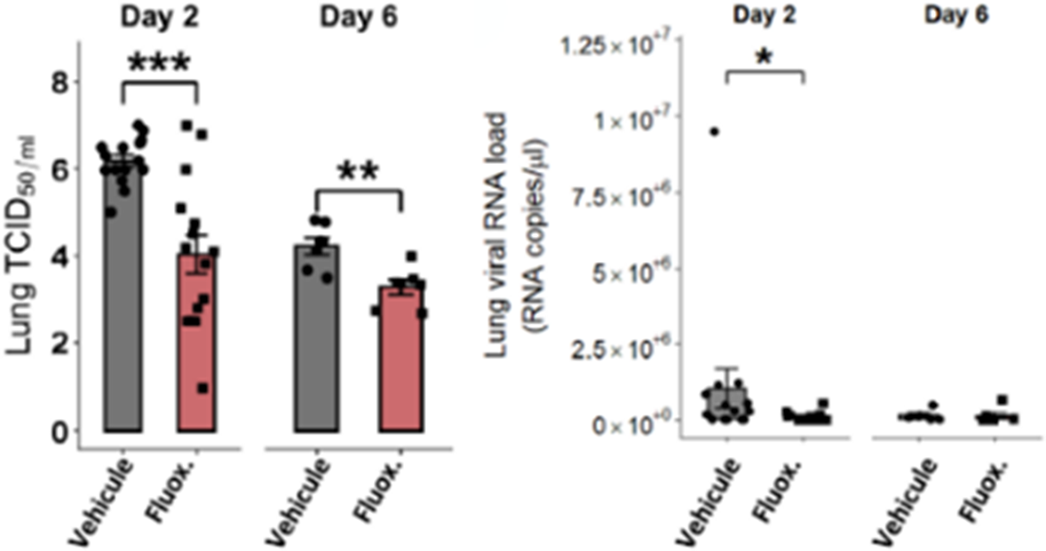
Image 2:
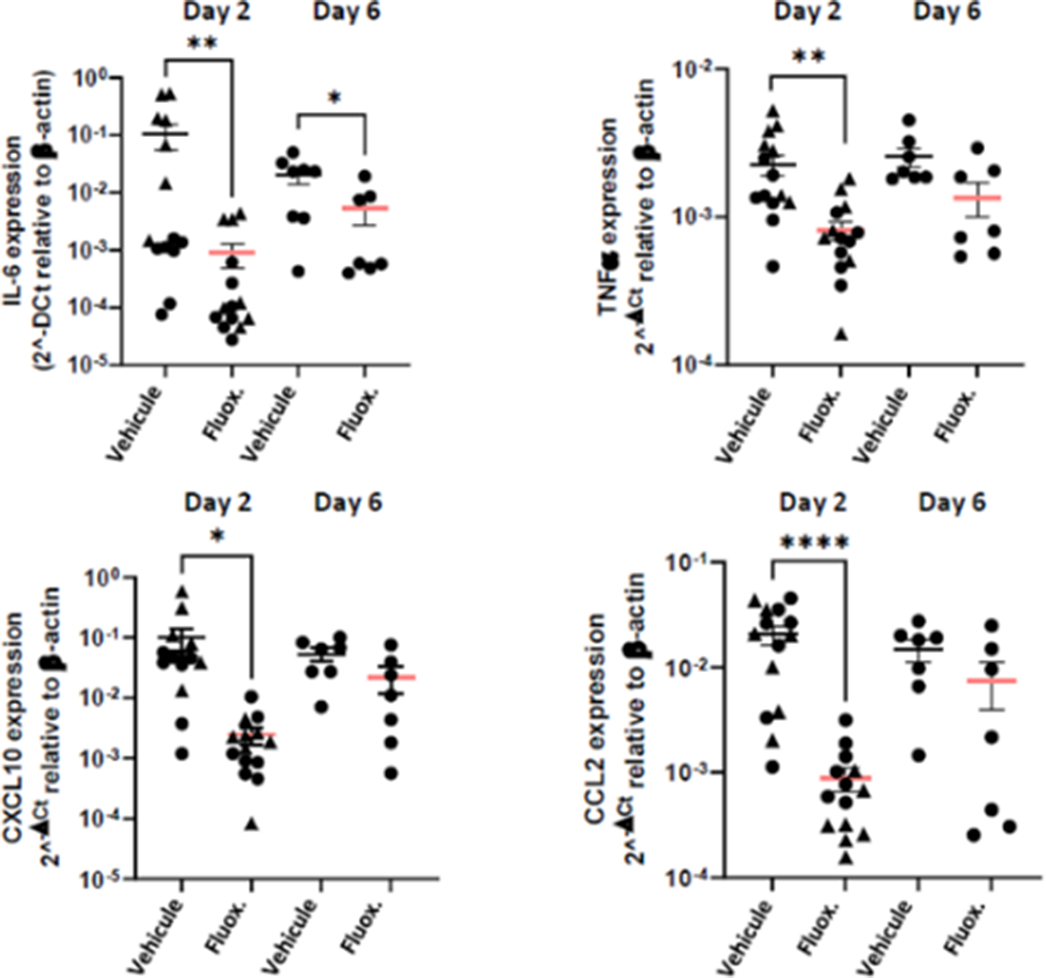
Image 3:
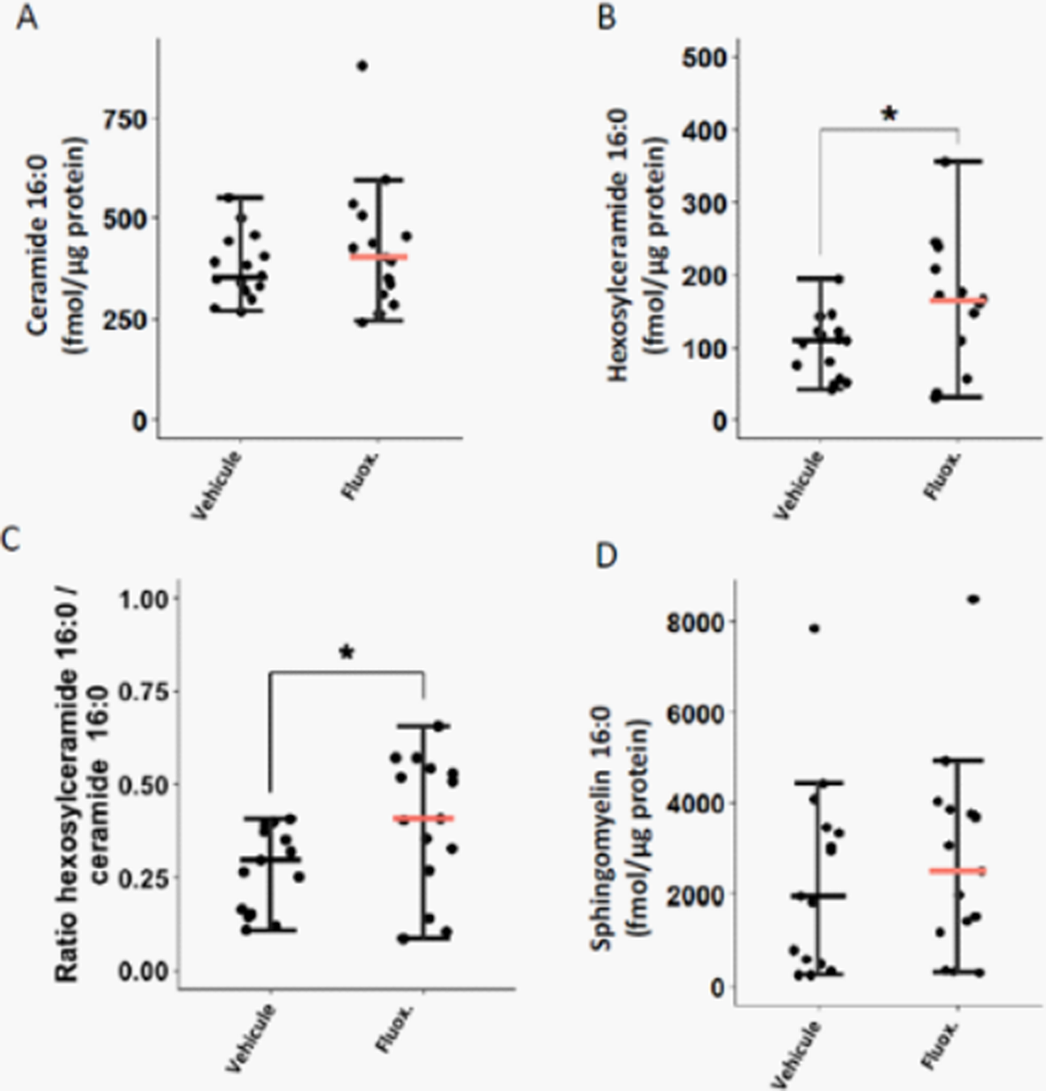 Conclusions
ConclusionsOur findings demonstrate the antiviral and anti-inflammatory properties of fluoxetine in a K18-hACE2 mouse model of SARS-CoV-2 infection, and its in vitro antiviral activity against variants of concern, establishing fluoxetine as a very promising candidate for the prevention and treatment of SARS-CoV-2 infection and disease pathogenesis.
Disclosure of InterestNone Declared
Antidepressant Use and Its Association with 28-Day Mortality in Inpatients with SARS-CoV-2: Support for the FIASMA Model against COVID-19
- N. Hoertel, M. Sanchez-Rico, J. Kornhuber, E. Gulbins, A. Reiersen, E. Lenze, B. A. Fritz, F. Jalali, E. Mills, C. Cougoule, A. Carpinteiro, C. Mühle, K. A. Becker-Flegler, D. R. Boulware, C. Blanco, J. M. Alvarado, N. Strub-Wourgaft, C. Lemogne, F. Limosin
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S118-S119
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
To reduce Coronavirus Disease 2019 (COVID-19)-related mortality and morbidity, widely available oral COVID-19 treatments are urgently needed. Certain antidepressants, such as fluvoxamine or fluoxetine, may be beneficial against COVID-19.
ObjectivesThe main objective was two-fold: (i) to test the hypothesis that the prevalence of antidepressant use in patients hospitalized with COVID-19 would be lower than in patients with similar characteristics hospitalized without COVID-19, and (ii) to examine, among patients hospitalized with COVID-19, whether antidepressant use is associated with reduced 28-day mortality. Our secondary aim was to examine whether this potential association could only concern specific antidepressant classes or molecules, is dose-dependent, and/or only observed beyond a certain dose threshold.
MethodsWe included 388,945 adult inpatients who tested positive for SARS-CoV-2 at 36 AP–HP (Assistance Publique–Hôpitaux de Paris) hospitals from 2 May 2020 to 2 November 2021. We compared the prevalence of antidepressant use at admission in a 1:1 ratio matched analytic sample with and without COVID-19 (N = 82,586), and assessed its association with 28-day all-cause mortality in a 1:1 ratio matched analytic sample of COVID-19 inpatients with and without antidepressant use at admission (N = 1482) (Figure 1).
ResultsAntidepressant use was significantly less prevalent in inpatients with COVID-19 than in a matched control group of inpatients without COVID-19 (1.9% versus 4.8%; Odds Ratio (OR) = 0.38; 95%CI = 0.35–0.41, p < 0.001) (Figure 2). Antidepressant use was significantly associated with reduced 28-day mortality among COVID-19 inpatients (12.8% versus 21.2%; OR = 0.55; 95%CI = 0.41–0.72, p < 0.001), particularly at daily doses of at least 40 mg fluoxetine equivalents (Figure 3). Antidepressants with high FIASMA (Functional Inhibitors of Acid Sphingomyelinase) activity seem to drive both associations.
Image:
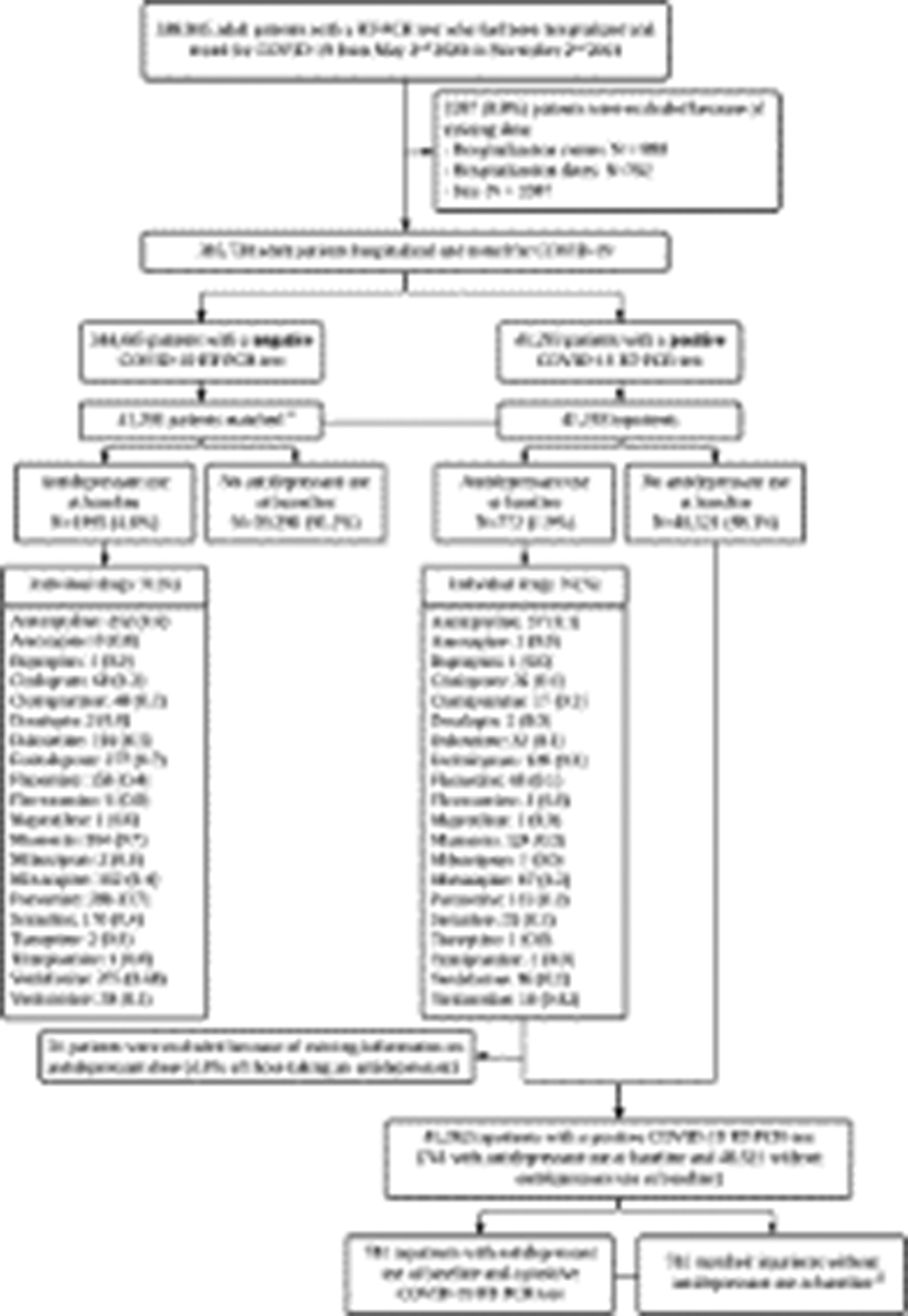
Image 2:
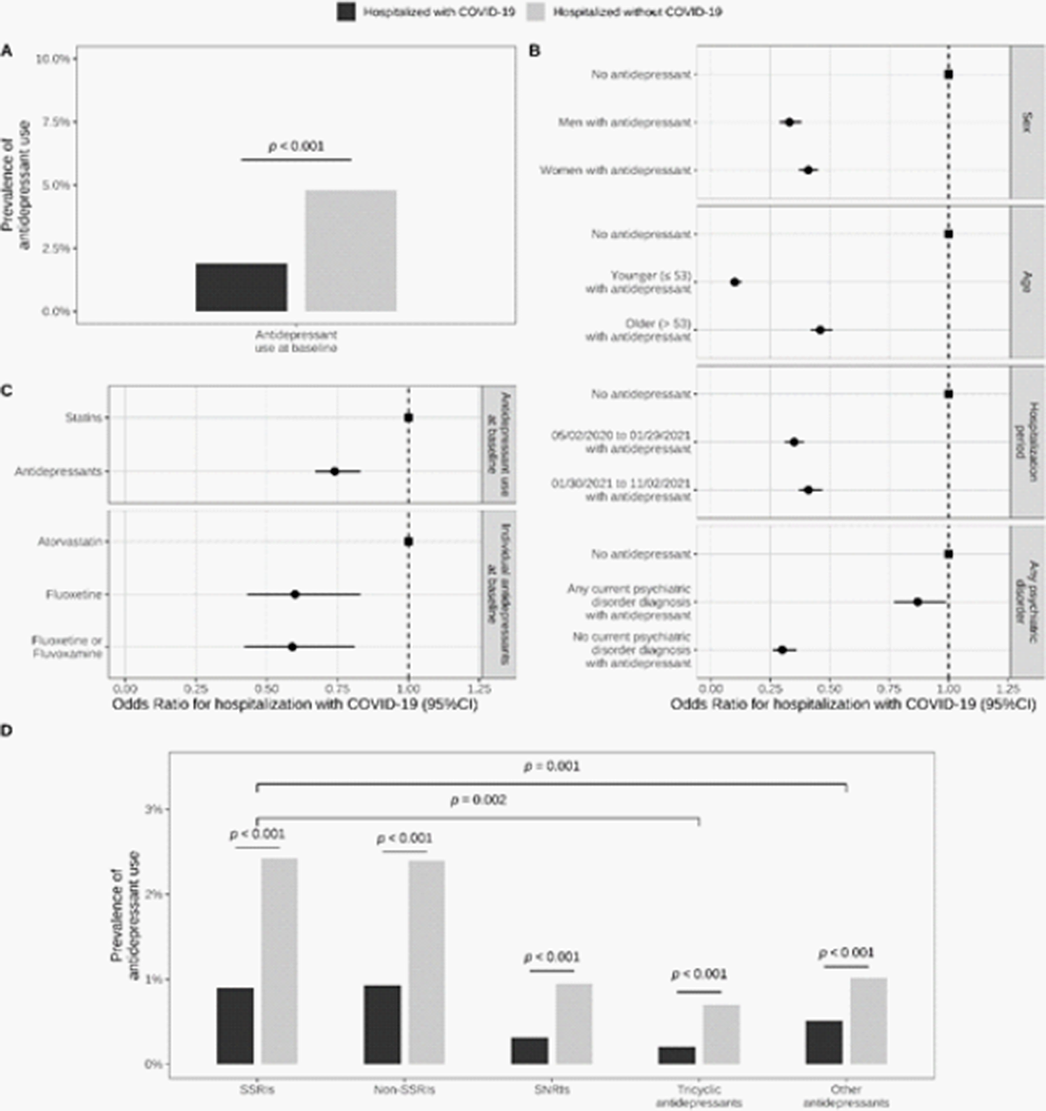
Image 3:
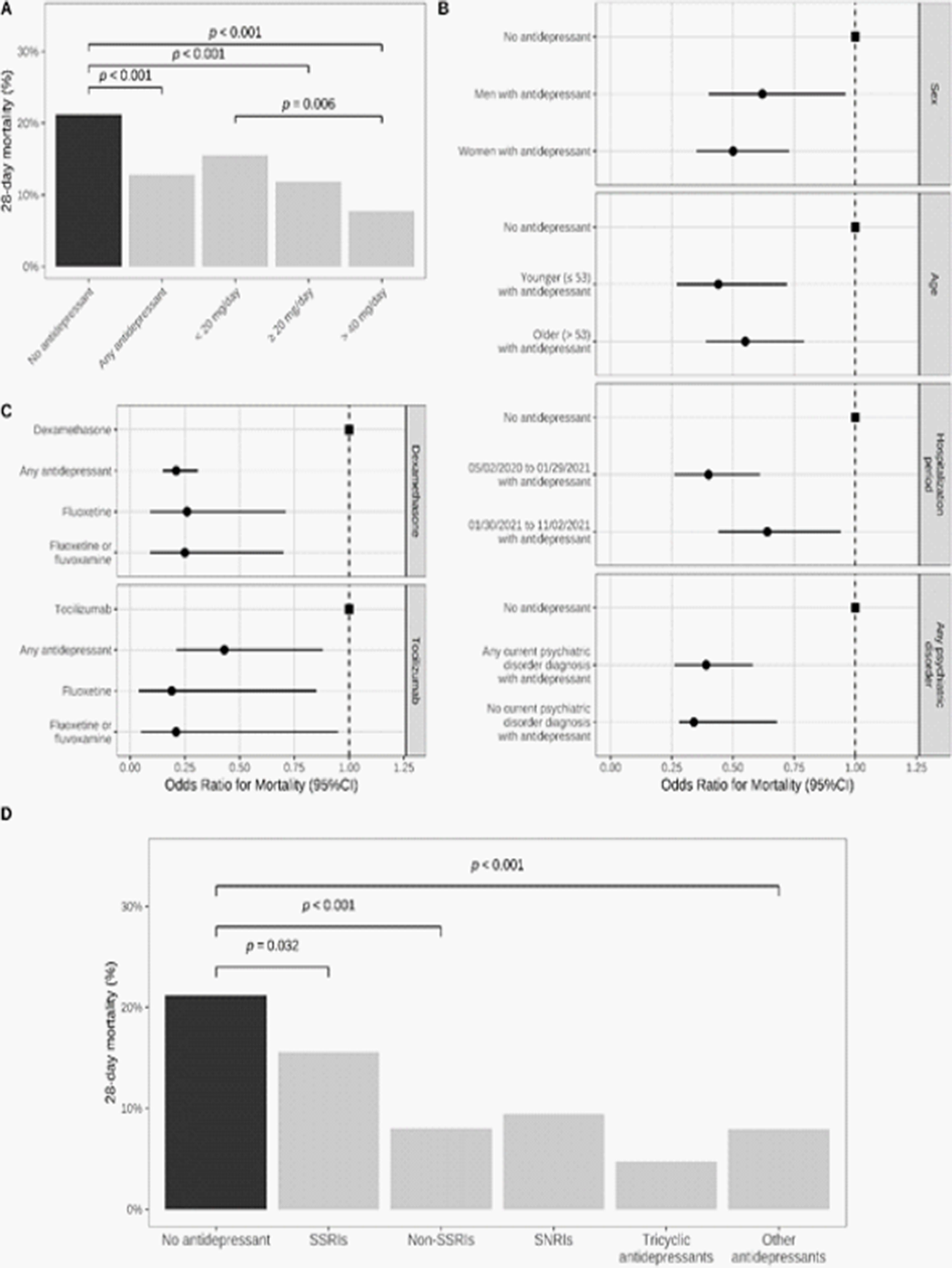 Conclusions
ConclusionsAntidepressant use is associated with a reduced likelihood of hospitalization in patients infected with SARS-CoV-2 and with a reduced risk of death in patients hospitalized with COVID-19. These associations were stronger for molecules with high FIASMA activity. These findings posit that prospective interventional studies of antidepressants with the highest FIASMA activity may be appropriate to help identify variant-agnostic, affordable, and scalable interventions for outpatient and inpatient therapy of COVID-19.
Disclosure of InterestNone Declared









